CY2027 Final Rule: A Simpler Program with Less Room for Error
Let’s have a conversation
CMS’s CY2027 Final Rule simplifies the Stars program but raises the stakes for performance. With fewer measures and greater concentration of weight, small performance gaps will have outsized financial impact, especially for plans near 4 Stars. CMS estimates $18B+ in payment reductions over the next decade, reinforcing that even incremental changes in performance now carry meaningful financial consequences.
CMS is accelerating a shift away from administrative measures toward those that directly reflect member experience and clinical outcomes. As process-focused measures are phased out, performance will be driven by how members experience care and whether that care leads to meaningful health improvement, not how well processes are documented. While the Reward Factor remains in place and the Health Equity Index reward will not be implemented, the overall direction signals increased weighting on performance in areas that matter most to beneficiaries, including access, experience and outcomes. The table below outlines the 11 measure removals and additions that bring this shift to life across the Stars program.
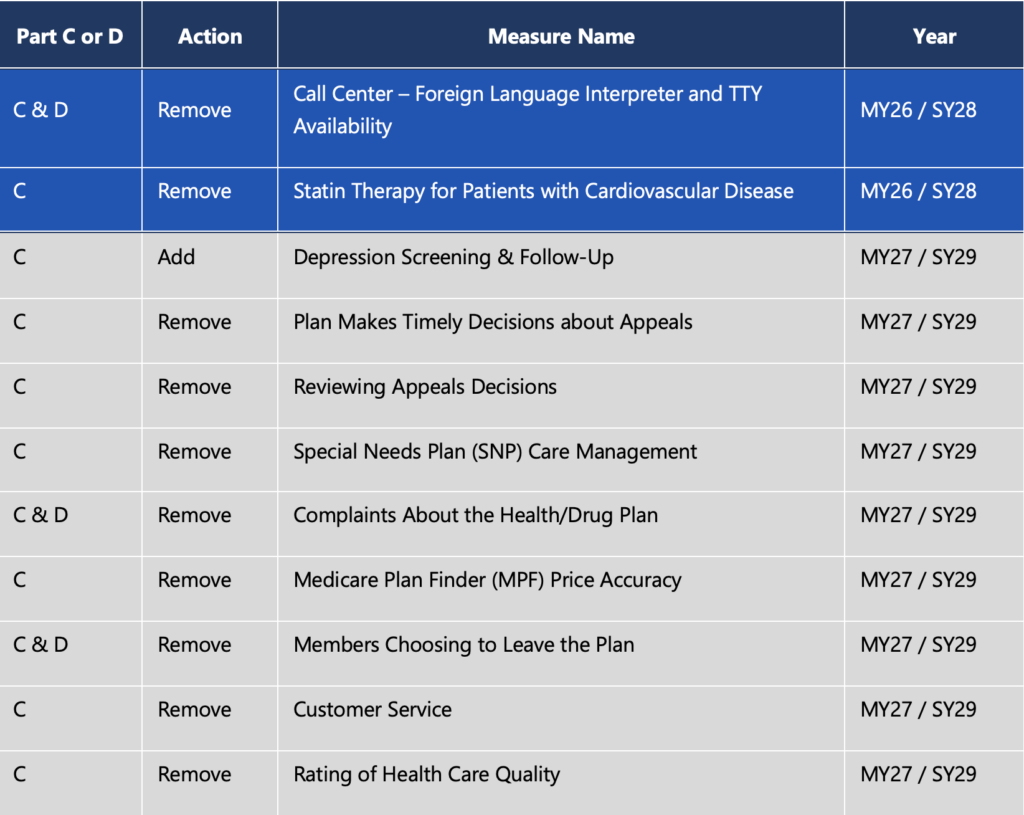
The removal of these measures will shift domain weighting. Starting in SY2029, HEDIS will carry the greatest influence on overall Star ratings, reinforcing that clinical outcomes, not process, will drive performance.
Domain Weights
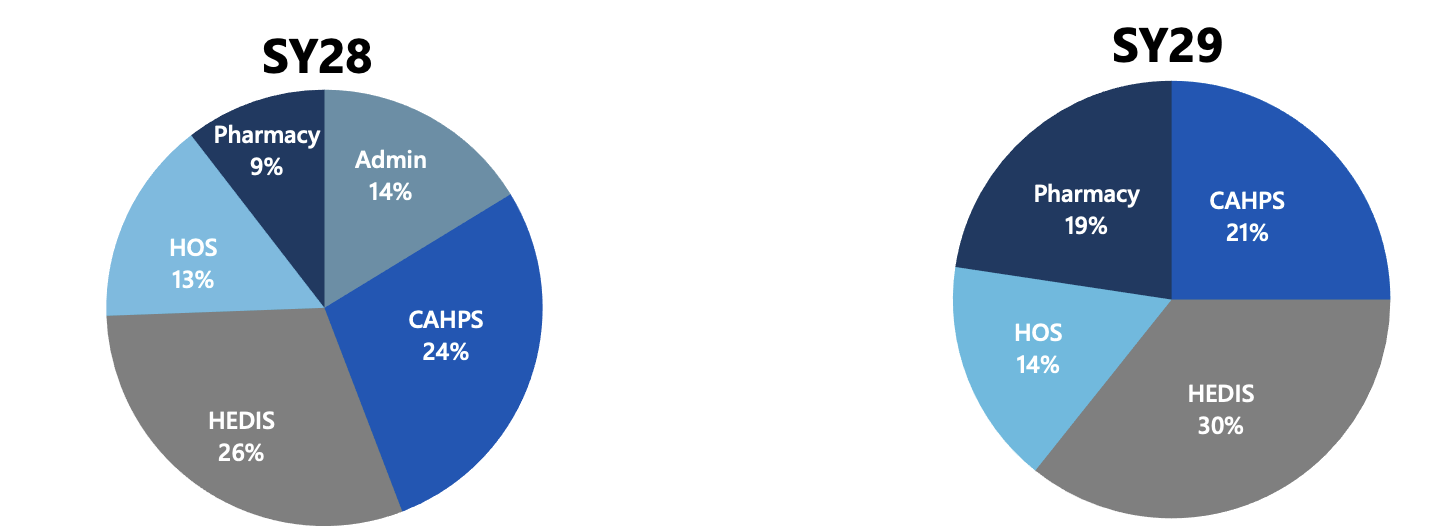
The result is a more streamlined program with less margin for error. With fewer measures acting as buffers, performance will be driven by a concentrated set of core metrics with fewer opportunities to offset underperformance.
What This Means Now and What to Do About It
Success in this environment will require more than closing gaps at the measure level. As CMS continues to concentrate weight on outcomes, performance will be driven by a smaller, more sensitive set of metrics with far less room for error.
Plans need to quickly shift from managing measures to managing populations:
- Which populations are actually driving performance?
- Where are outcomes breaking down across the member journey?
- Are interventions targeted or broadly deployed with limited impact?
At the same time, execution becomes more complex, not less.
Stars performance is no longer owned by a single team; it’s produced across the organization. Performance depends on how well clinical operations, network strategy, pharmacy and member experience work together to drive outcomes. Gaps in alignment across these areas will show up quickly and financially.
CMS is also moving toward greater direct accountability. While certain measures (e.g., Appeals) are rolling out of Stars, they remain subject to audit and monitoring. The buffer that Stars once provided is shrinking. Performance, compliance and financial outcomes are becoming more tightly linked.
The result is a near-term reality many plans are already feeling:
- You still need to deliver on current-year performance
- While simultaneously redesigning your strategy for what’s next
- With limited resources, increasing financial pressure and no clear “extra capacity” to do both
Where ProspHire Can Help
Leading plans are already shifting their Stars strategy: moving from measure-level optimization to enterprise execution.

We partner with plans to move beyond strategy and into action:
- Prioritizing what Matters Most - aligning investments and interventions to the populations and measures that drive performance
- Turning Data into Action - understanding not just where gaps exist but why and what to do about them
- Driving Cross-Functional Alignment – connecting clinical, pharmacy, experience and operations to deliver results
- Integrating Stars Efforts End to End – bringing CAHPS, HEDIS and Part D into a cohesive, member-focused approach
- Executing and Sustaining Change - supporting implementation and long-term adoption so strategies deliver lasting results
This is not a moment for theoretical strategies or incremental adjustments. It requires focused prioritization, strong partnership and disciplined execution. In a program with fewer measures and higher stakes, performance won’t be determined by strategy. It will be determined by execution.
© 2026 ProspHire, LLC. All Rights Reserved / Terms of Use / Privacy Policy







