Star Year 2023 Data Insights
Let’s have a conversation
On October 6th, 2022, the Centers for Medicare and Medicaid (CMS) released the official Star Year 2023 Data - including contract and measure level detail to the public. As we’ve talked about for some time now, the industry did observe a great Stars recession with average ratings plummeting year over year and returning to pre-pandemic levels (SY2020). With many important regulatory changes already in place and several on the way (Tukey Outlier Deletion), Health Plans can anticipate more disruption in the marketplace.
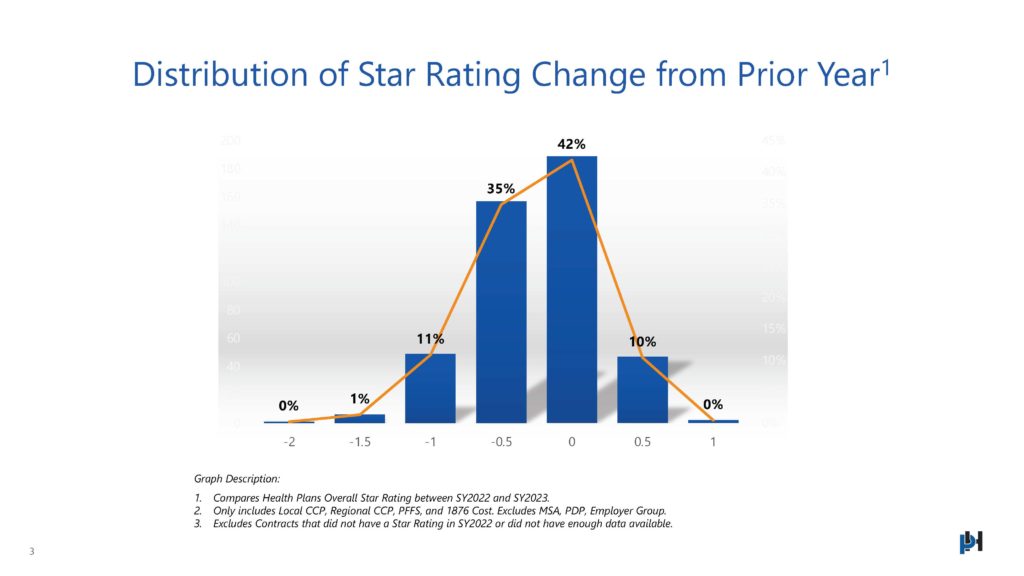
Distribution of Star Rating Change from Prior Year
Nearly 20% of Health Plans experienced a drop out of the Quality Bonus Payment (QBP) range in SY2023. Last year, about 70% of contracts achieved the QBP whereas in 2023 only about half of contracts got the QBP. This drop will put added financial pressure on health plans to achieve cost savings either through improved medical management or enhanced revenue capture. More importantly, this negative shift represents the new Stars reality, where CAHPS and Member Experience performance will drive the bulk of the marketplace and will force plans to invest more time and effort into benefits, personalized member experiences, and improved operational excellence.
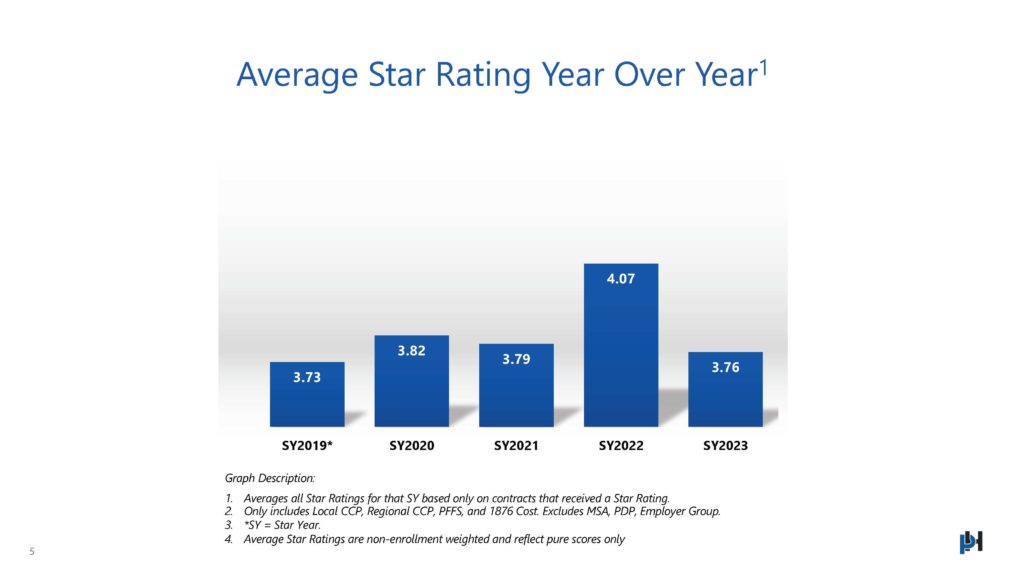
Average Star Rating Year Over
Since the programs’ inception, Star Ratings have steadily increased year over year. Due to COVID guardrails and other “better of” protections, SY2022 was the highest on record and for many, was quite anomalistic. The SY2023 drop off was quite precipitous, with average ratings falling to near pre-pandemic levels. What does this all mean? It’s hard to say in the long run, but we cannot discount the impact that Member Experience and CAHPS will have on the programs overall average rating for the foreseeable future. Perhaps with these weighting changes, the program will see a ‘leveling off’ for the next few years as average scores remain neutral. In any case, those Health Plans that saw massive drop offs in scoring will have plenty of opportunity to rescue their scores in SY2024 and beyond.
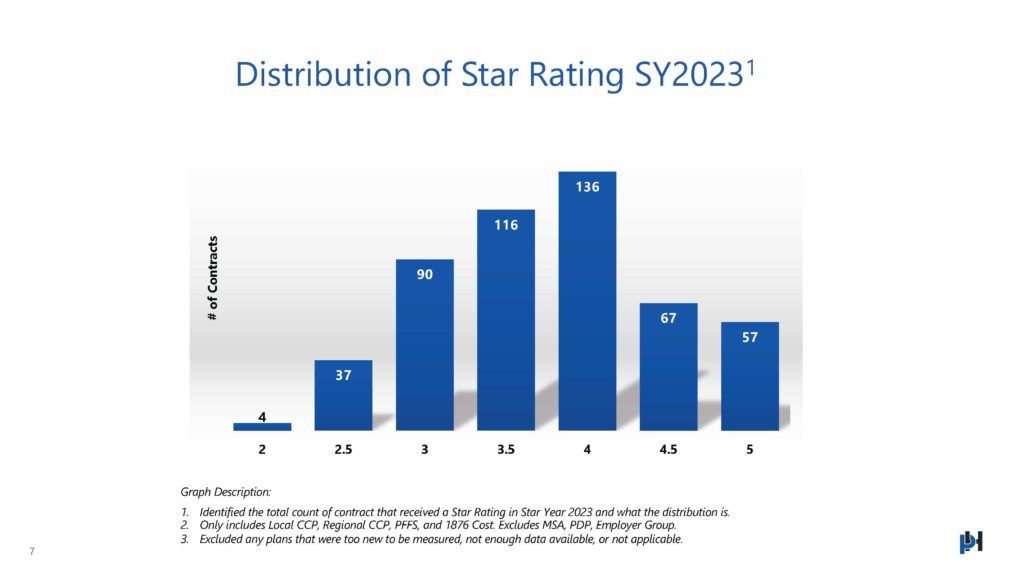
Distribution of Star Rating SY2023
When analyzing the distribution of Star Ratings for SY2023, the biggest takeaway are the tail ends of the distribution. We saw a big drop off in 5-Star plans (year over year) and a massive increase in 2- and 2.5-Star plans (year over year). With almost 50% of plans facing a drop in Star Rating year over year, the distribution of ratings returned to a somewhat more normal distribution.
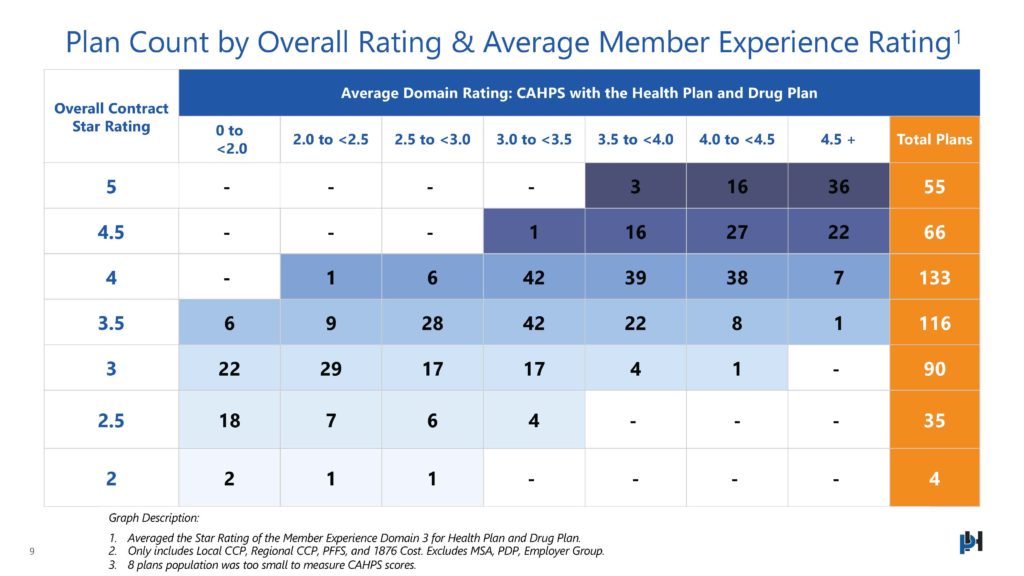
Plan Count by Overall Rating & Average Member Experience Rating
In SY2023, CMS adjusted the weighting of CAHPS and Member Experience measures to account for ~60% of the Overall Star Rating, shifting Health Plan’s focus away from majority gap closure efforts to putting member experience at the forefront of strategies. 254 contracts were able to achieve a 4.0 Star Rating with this adjustment in the Star rating landscape. Approximately 60% of contracts with 4.0 Stars or greater, scored >=4.0 Stars in the CAHPS Domains. This further emphasizes that CAHPS/Member Experience are major drivers in overall contract rating performance and failing to succeed in those areas will hurt your plan performance. Bottom line, 70% of plans with <4.0 Stars in CAHPS were not able to achieve the QBP and did not receive 4.0+ Stars at the contract level.
ProspHire
216 Blvd of the Allies, Sixth Floor
Pittsburgh, PA 15222
412.391.1100
[email protected]
Quick Links
© 2024 ProspHire, LLC. All Rights Reserved / Terms of Use / Privacy Policy









