Leveraging Evidence-Based Interventions to Address Population Health
Let’s have a conversation
As payers and providers continue to manage the impact of COVID-19 on their populations, social determinants of health (SDOH) remain a focus for improving population health. Addressing SDOH has become even more vital as the pandemic had a disproportionate effect on the most vulnerable populations who are also greatly impacted by SDOH-related issues. While it remains at the forefront of strategy across the healthcare industry, it is imperative that interventions targeting SDOH are measurable and evidence-based to draw insights into conclusive results. In doing so, organizations will be better equipped to implement successful SDOH initiatives driving improved health outcomes.
What Are the Key Areas of SDOH?
SDOH describes the conditions in which people are born, live, learn and play, among other things and impact a wide range of health, functioning and quality of life concerns.[1] The Centers for Disease Control has identified five key areas of focus including healthcare access and quality, economic stability, education access and quality, neighborhood and built environment, and social and community context.[2] There is consensus regarding the need for consideration of these factors when measuring health; however, success has been varied with decision makers often crafting solutions from afar and without local and member-level input or data to support their efforts. While traditional healthcare services remain vital to measuring health, it is only one piece in a complex web of factors that impact health costs and outcomes. Studies show that social determinants can have a greater impact than healthcare or lifestyle choices in influencing a person’s health with some showing that they can account for as much as 80% of health outcomes.[3] This includes food insecurity, job security, education, among others; however, efforts to address these issues have largely been unsuccessful. There are programs across the country targeting these various issues and it is important that they be measured for impact and success.

A common SDOH highlighting this issue is food security, defined as a household-level economic and social condition of limited or uncertain access to adequate food.[1] Food security can be temporary or long term and is influenced by various social factors including job security, disability and income, among others. When crafting interventions to target food security, it’s important to think broadly about the surrounding factors that influence it. Access to food is crucial, but so is consideration of the transportation needed to acquire that food (or lack thereof) and an intervention that targets food distribution without consideration of the related factors is doomed to fail. One organization working to address food security is Feeding America, which manages a nationwide network of food banks and other community-based agencies to feed more than 46 million people yearly.[2] The organization has developed a Framework to mitigate the implementation of unhelpful or unsuccessful interventions targeting food security[3]
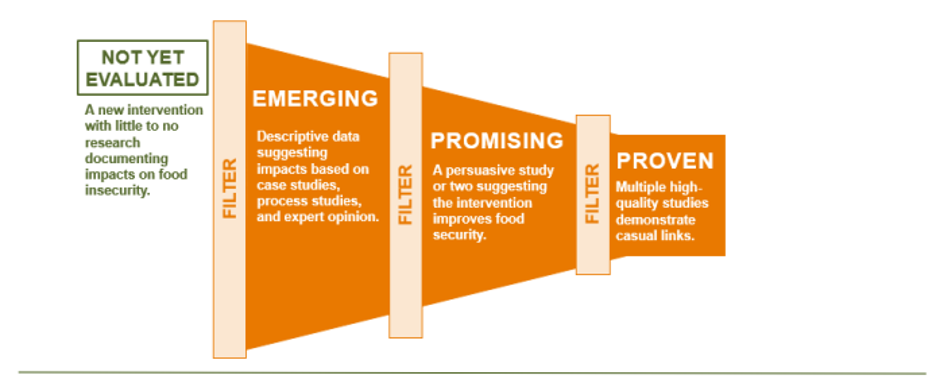
Feeding America highlights the Supplemental Nutrition Assistance Program (SNAP) as an example of a ‘proven’ SDOH framework – one that has demonstrated consistent positive improvement to accessing healthy food through multiple studies. It has accomplished this through local networks of food banks, despite being a national program. This local approach allows for tailored outreach activities, utilizing community networks and unique language and cultural needs to deliver services that are useful for the communities needing it the most.[1]
Despite this, it is important to note that while the intervention itself may be evidence-based in its implementation, it is not immune to external factors that could limit its effectiveness. The framework also takes into account those conditions that could impact an intervention’s success such as the high cost of food. Considering the rising food prices in 2022, approximately 10% higher according to the USDA, this would have a direct impact on a program like SNAP’s success, as the benefits are not regularly adjusted to reflect variation in food costs or cost-of-living. Therefore, when evaluating an intervention on its effectiveness in addressing SDOH, it is imperative to remember that they don’t exist in isolation and are continuously impacted by our changing world.
There is a growing recognition that building strategies that incorporate SDOH are beneficial for both providers and payors. These initiatives provide opportunities to address population health needs in communities across the country, which can improve care for members while reducing costs, if done correctly. To accomplish this, it is essential that SDOH interventions be evidence-based and both collaborative and customized to local communities, enabling organizations to increase the effectiveness of their initiatives while improving care for the most vulnerable populations.
How Can ProspHire Help?

At ProspHire, we want to ensure your programs have the greatest impact on members and patients, while simultaneously addressing the disparities that exist across our communities. Our team’s extensive knowledge in this topic can help your organization optimize strategies and deliver effective programs that support the most vulnerable populations. We understand the challenges and solutions to drive change through social determinants with a focus on your unique member and patient needs. Reach out today for more information to partner in this important work.
References
- https://health.gov/healthypeople/priority-areas/social-determinants-health
- Healthy People 2030, U.S. Department of Health and Human Services, Office of Disease Prevention and Health Promotion. Retrieved [May 18, 2023], from https://health.gov/healthypeople/objectives-and-data/social-determinants-health
- https://www.rwjf.org/en/insights/our-research/2019/02/medicaid-s-role-in-addressing-social-determinants-of health
- https://health.gov/healthypeople/priority-areas/social-determinants-health/literature-summaries/food-insecurity
- [1] https://www.feedingamerica.org/sites/default/files/research/hunger-in-america/hia-2014-executive-summary.pdf
- https://www.feedingamerica.org/sites
- https://www.feedingamerica.org/sites/default/files/2018-10/snap-outreach-evaluation.PDF
© 2026 ProspHire, LLC. All Rights Reserved / Terms of Use / Privacy Policy







