Soaring to New Health: Healthcare Uncovered Series
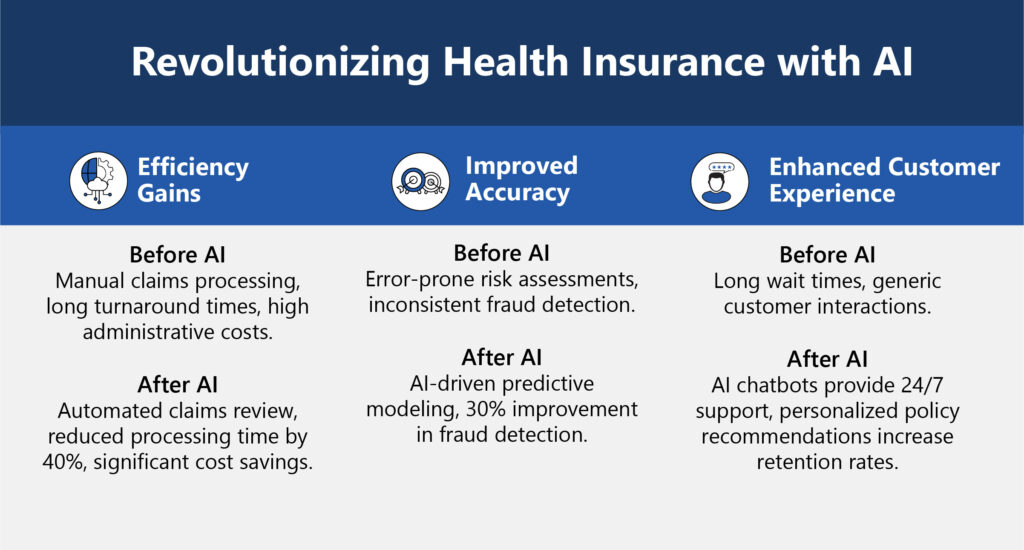
Welcome to the Healthcare Uncovered Podcast Series– your front-row seat to the future of healthcare. In this exclusive blog series, we spotlight expert insights and real-world strategies from ProspHire’s Soaring to New Health podcast. Each episode takes a deep dive into a distinct area of the healthcare ecosystem, from the rise of cloud-based dental software to unlocking Medicare Stars success, optimizing Medicaid and navigating the ever-changing ACA marketplace. Whether you’re a provider, payer or industry leader, these conversations are designed to inform, inspire and empower you to drive meaningful change. Need a quick overview? Click on the series highlights infographic to the right.

Explore the full series below and uncover the innovation shaping healthcare today.
The Modern Dental Practice – Software to Believe In
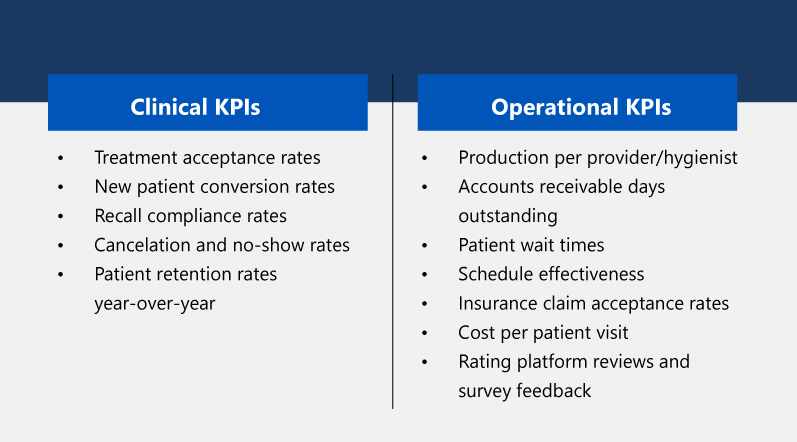
Revolutionizing Dental Care Through Technology
The dental industry is evolving, and cloud-based solutions are leading the charge. In this episode, we dive into the future of dental practice management software and how innovations are helping dental organizations scale, optimize operations, and improve patient care.
Our experts discuss the impact of cloud technology, how it enhances workflow efficiency and why leading dental practices are making the switch from legacy systems. If you’re looking to streamline practice management and improve operational outcomes, this episode is a must-listen!
Tune in now to discover how technology is transforming dental care!
Stars Performance – Unlocking 5-Star Success
How Health Plans Can Improve Quality and Performance
Achieving a 5-Star rating is no small feat, but it’s essential for health plans aiming to deliver high-quality care while maximizing reimbursement. In this episode, we break down the critical factors behind Stars success, from improving member engagement to optimizing HEDIS and CAHPS performance.
Our experts share best practices for navigating CMS guidelines, addressing key challenges in Stars improvement and driving meaningful quality outcomes. If you’re looking to enhance your health plan’s Star rating, this conversation provides actionable insights you won’t want to miss.
Listen now and take your Stars strategy to the next level!
Medicaid Strategy – Enhancing Access and Efficiency
Innovative Approaches to Medicaid Optimization
Medicaid plays a crucial role in providing healthcare access but navigating its complexities requires strategic expertise. In this episode, we explore how health plans and providers can enhance Medicaid quality, control costs and improve member experiences.
We cover key topics like Medicaid HEDIS optimization, addressing health disparities and integrating new technologies to streamline processes. With rising demands on Medicaid programs, this discussion is essential for healthcare leaders looking to drive innovation and efficiency in Medicaid services.
Tune in to explore cutting-edge strategies for Medicaid success!
The ACA Marketplace – What’s Next?
Navigating Risk Adjustment and Market Trends
The Affordable Care Act (ACA) marketplace continues to evolve and insurers must stay ahead of changing regulations, risk adjustment policies and enrollment trends. This episode takes a deep dive into the challenges and opportunities in the ACA landscape.
Our discussion highlights risk adjustment transfer payments, how insurers can optimize financial performance and the impact of policy shifts on healthcare access. Whether you’re an insurer, policymaker or healthcare leader, this episode unpacks the latest insights shaping the ACA marketplace.
Listen now to stay informed on the future of ACA and risk adjustment!